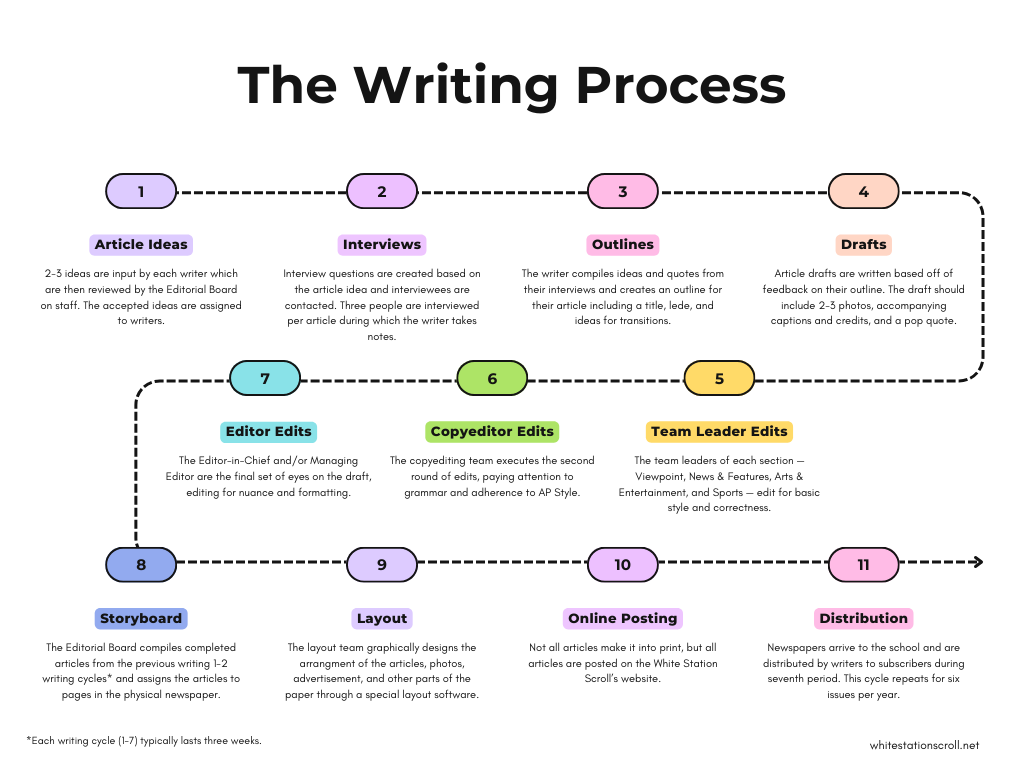
The science behind the COVID-19 vaccines
Similar to other vaccines, the mRNA COVID-19 vaccine operates by allowing the immune system to generate antibodies against the production of the virus. There is minimal risk of DNA damage or other long term effects, though short term side effects are common after receiving the vaccine.
Receiving a vaccine for the COVID-19 disease as soon as possible is an important way to protect from the virus. As of February, more than 40 million doses of the vaccine have been administered to Americans. The pharmaceutical company Pfizer and the biotechnology company Moderna have both produced mRNA vaccines that are being distributed to the public. Both vaccines have been authorized for emergency use (EUA) by the U.S. Food and Drug Administration.
The COVID-19 vaccine is understood best by looking at the ways in which the human body fights illnesses in general.
“It is important to understand…[COVID-19] is caused by a virus, and not a bacteria,” Harry Kochat, Ph.D, Director of Operations at
the Plough Center for Sterile Drug Delivery Solutions at the University of Tennessee Health Sciences Center, said. “You cannot kill a virus because the virus itself is not a living organism that needs a host to be active.”
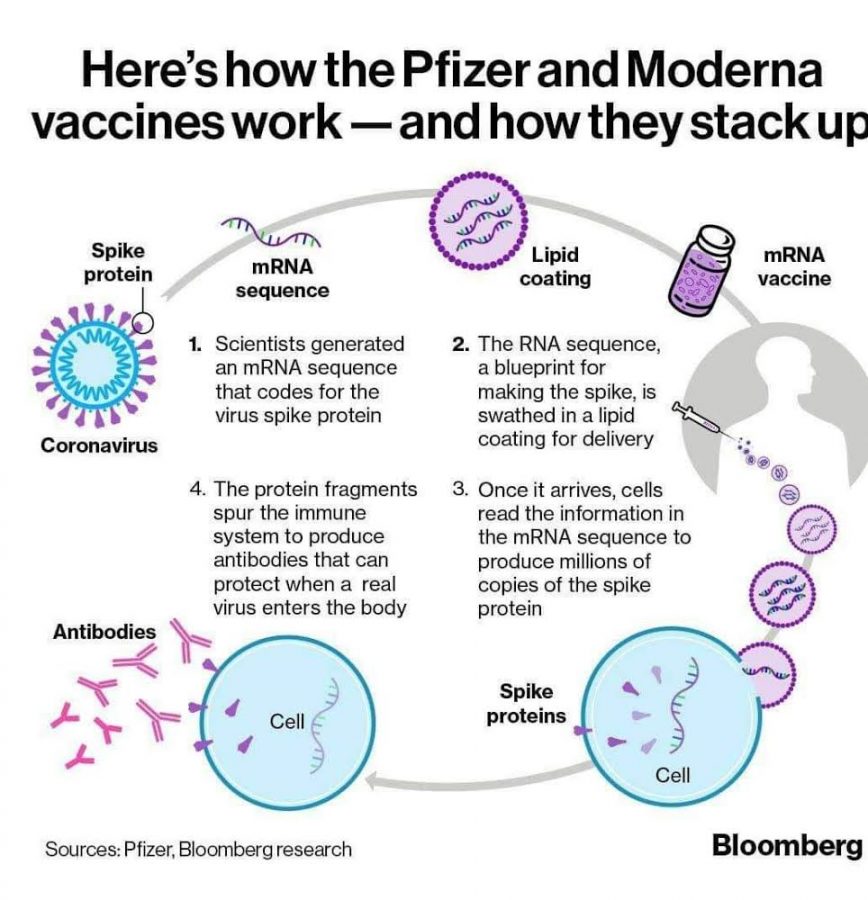
The primary type of COVID-19 vaccine distributed in the United States is the messenger RNA (mRNA) vaccine. mRNA vaccines, according to the Center for Disease Control (CDC), work mostly by generating antibodies from a genetic material known as mRNA. It should be noted that because the mRNA does not enter the nucleus of the cell, there are no risks of the vaccinated person’s DNA changing.
“The spike protein fragments that the mRNA vaccine helps create is what helps your body generate antibodies and protects from the virus,” Kochat said. “The receptor sites are called spike proteins. …When the produced antibodies match those receptor sites and can bind onto the receptor sites, that is where the virus [will be killed]”
The encapsulated mRNA produces spike proteins. Once the spike proteins get out of the cell, these help T-cells and B-cells, which are cellular components of the immune system, to generate the antibodies.
“Messenger RNA has the ability to control, encode and decode, and it has the ability to regulate genetic code best,” Kochat said. “T-cells and B-cells actually help to develop what we call antibodies, and they suppress that piece of the RNA that is introduced into your system. It helps the body to develop immunity against the anticipated activity of the virus.”
One common fear about receiving the COVID-19 vaccine is the side effects that may follow shortly afterwards. According to the CDC, “While some people don’t have any side effects after getting a COVID-19 vaccine, many people will have mild side effects after COVID-19 vaccination, like pain or swelling at the injection site, a headache, chills, or fever.” However, receiving side effects after getting the vaccine may have positive indications as well.
“Getting those side effects or any mild reaction is the potential indication that the vaccine is taking effect inside your body,” Kochat said. “[Some people] have the misconception that the virus can mutate DNA once it has been released into your body, but this is not true. What it is actually doing is producing is the proteins that will serve as the recognition sites for the T-cells and B-cells, which produce the antibodies that protect you.”
Another concern posed by many who have received the vaccine is the possibility that COVID-19 may have developed regional strains, similar to influenza. However, the advanced nature of the vaccine mitigates this risk as well. In mRNA technology, an engineered fragment of the COVID-19 virus encoded with the spike protein coding is inserted. This means that the chances of the virus taking form inside the human body are close to none.
“[Mutations] can happen. That is why the new technology has more benefit over the conventional way of making the vaccine, because the conventional vaccine would only be specific to a certain strain of the virus,” Kochat said. “Now, this new mRNA technology can cover other variants [of COVID-19] because these spike proteins have many more receptors that can attach to the antigens of this virus.“
These shots have two doses, separated by several days. For patients taking the Pfizer-BioNTech vaccine, the two-dose series is separated with 21 days in between, and for those taking the Moderna vaccine, the two-dose series is separated by 28 days.
“The reason [for the two-dose series] is that 50% of immunity is created in the period between the two doses” Kochat said..“This immunity may go down, but then the booster shot after is what elevates [the immunity] and keeps the level stable for a period of time. How long is yet to be determined”
Since both vaccines have been authorized for emergency use, Pfizer and Moderna have reported that their vaccines show about 95% efficacy at preventing both mild and severe symptoms of COVID-19.
“…It doesn’t mean that 95% of people are 100% protected, it is based on the clinical trial that states that 95% of people can be prevented from entering the serious stage [of COVID-19],” Kochat said. “The level of antibodies… vary from one person to another because it depends on how immunity is developed inside your body. How much T-cells and B-cells are available…it varies.”
Though the COVID-19 vaccine is effective overall, it is important to ensure that other protective measures are still taking place. Wearing a mask in public and practicing social distancing are key to reducing the spread as the vaccine becomes more available to all.
“Even if you have immunity… you can still be a spreader to other people without knowing,” Kochat said. “So that’s why you should still wear a mask until at least 90% of your community receives the vaccine.”
Communication between patients and their physicians is vital to ensuring the best experience when taking both doses of the vaccine.
“[Physicians] must ensure that the vaccine is stored and transported at the temperature that was recommended,” Kochat said. “…Patients should make sure to be honest and open with their doctor about any preexisting conditions, asking any questions they may have.”
Your donation will support the student journalists of White Station High School. Your contribution will allow us to purchase equipment and cover our annual website hosting costs.